A Comprehensive Overview of Cognitive Behavioral Therapy: The Science Behind Mind and Behavior
A Comprehensive Overview of Cognitive Behavioral Therapy: The Science Behind Mind and Behavior
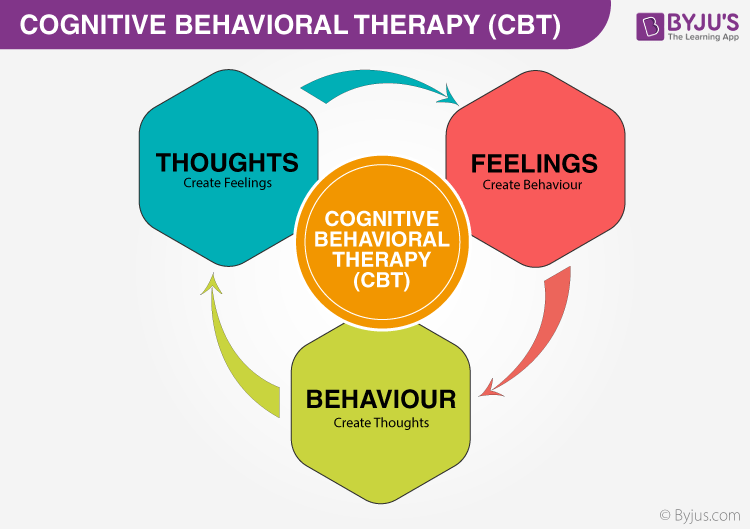
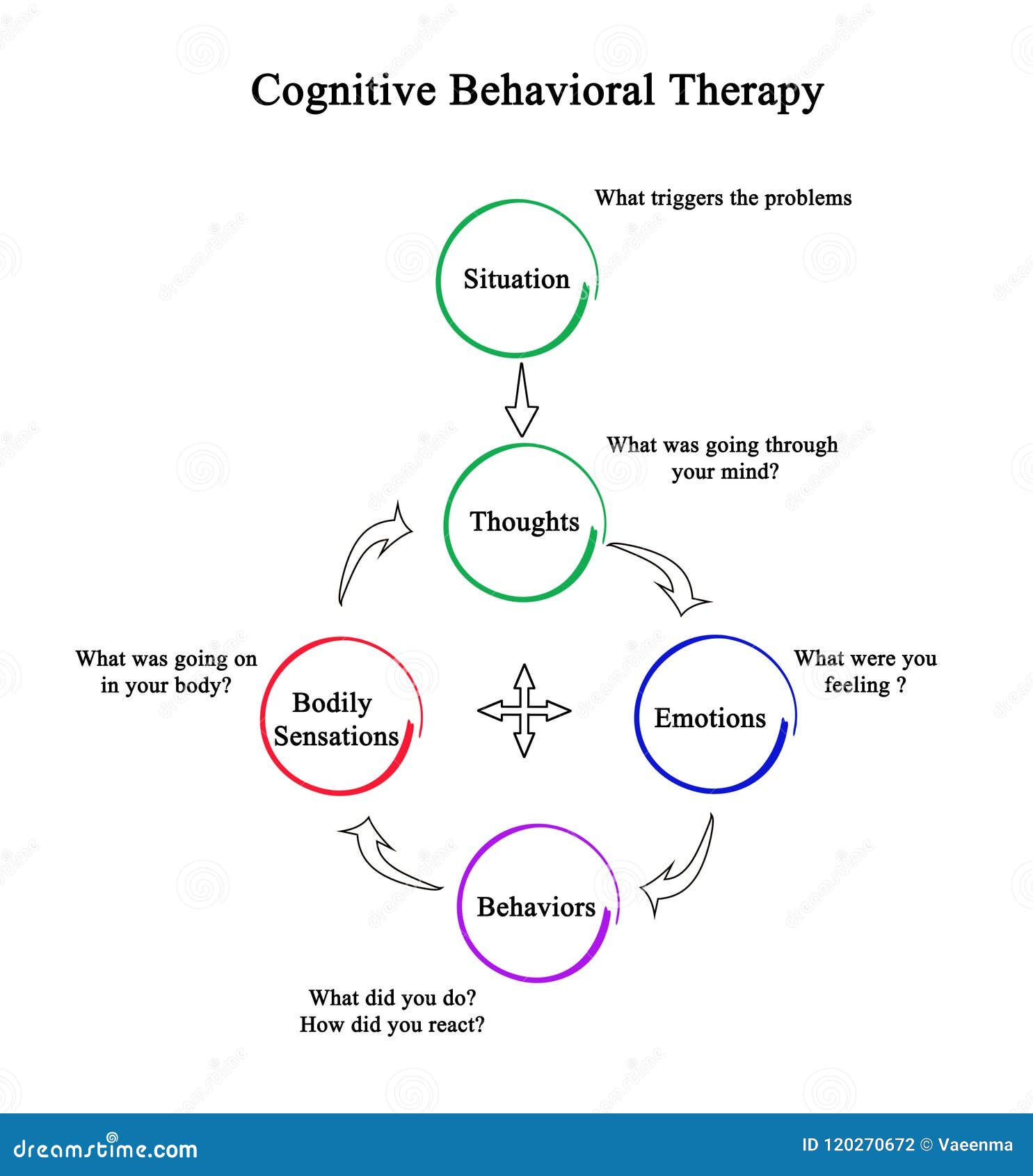
Oliver Jordan Ressler offers a thorough examination of Cognitive Behavioral Therapy (CBT), revealing how it bridges psychological insight and practical intervention. Rooted in the principles that thoughts, emotions, and behaviors are deeply interconnected, CBT stands as one of the most empirically validated therapeutic modalities of modern psychiatry. This overview distills the core mechanisms, clinical applications, and empirical support underpinning CBT, positioning it not as a fleeting trend, but as a foundational pillar in behavioral medicine.
At its essence, Cognitive Behavioral Therapy operates on a simple yet powerful premise: maladaptive thinking patterns fuel emotional distress and dysfunctional behaviors. By identifying and restructuring these cognitive distortions, CBT equips individuals with tools to challenge negative beliefs, modify unhelpful habits, and build resilience. “CBT doesn’t just treat symptoms—it changes the way people think and act,” observes clinical psychologist and CBT specialist Dr.
Elena Park. “It’s about rewiring thought patterns to create lasting psychological change.”
Central to CBT’s methodology is its structured, goal-oriented framework. Unlike open-ended psychoanalysis, CBT follows a time-limited, collaborative approach where therapists and clients work together to define specific objectives.
Sessions typically involve structured exercises such as:
- Cognitive restructuring: challenging irrational or distorted thoughts (“I always fail”) through evidence-based questioning.”
- Behavioral activation: scheduling meaningful activities to counteract depression-related withdrawal.”
- Exposure therapy: gradual, controlled confrontation of feared situations to reduce anxiety.”
- Problem-solving training: developing stepwise strategies to manage real-life stressors.”
Security in CBT’s reputation stems from its robust scientific foundation. Unlike treatments grounded solely in theoretical models, CBT relies heavily on randomized controlled trials (RCTs), neuroimaging studies, and longitudinal data. Neurobiological research supports its impact: fMRI scans reveal that post-CBT participants exhibit measurable changes in prefrontal cortex activity, the brain region responsible for emotional regulation and cognitive control.
“This isn’t just talk therapy—it’s neuroplasticity guided by intention,” notes Dr. Marcus Lin, a neuroscience researcher specializing in psychotherapeutic outcomes.
One of CBT’s distinguishing strengths lies in its adaptability across populations and settings. While originally developed for Western, adult patients, modern CBT iterations—such as Dialectical Behavior Therapy (DBT) for borderline personality disorder, Cognitive Processing Therapy (CPT) for trauma, and youth-focused CBT—have expanded its reach.
School-based programs now integrate CBT techniques to address adolescent anxiety and behavioral challenges, while digital platforms deliver accessible, evidence-based modules through apps and online modules, broadening impact to underserved communities.
Despite its strengths, CBT is not universally applicable. Some individuals may struggle with the active, self-reflective nature of the therapy, particularly those experiencing severe dissociation or cognitive impairments.
In such cases, hybrid models incorporating mindfulness or pharmacologic support often enhance outcomes. “Flexibility within evidence-based practice is key,” emphasizes leading CBT researcher Dr. Ana Torres.
“Success depends not on rigid doctrine but on tailoring intervention to the individual’s needs.”
Cost-effectiveness further strengthens CBT’s role in public health systems. Compared to long-term psychotherapy, CBT’s typical 12–20 session framework reduces both financial burden and treatment dropout rates. Health economists estimate that every dollar invested in CBT yields long-term savings by lowering relapse rates and associated healthcare utilization.
This pragmatic advantage has prompted global adoption, from the UK’s National Health Service to community clinics in low-resource regions.
The cultural resonance of CBT stems from its universal appeal: it empowers agency amid adversity, offering hope through demonstrable change. “People want to understand why they feel what they feel,” says Ressler.
“CBT doesn’t tell them who they are—it gives them actionable ways to grow.” As neuroscience deepens our understanding of mind-body dynamics, CBT continues to evolve, incorporating new insights from behavioral economics, social psychology, and digital health innovation.
In sum, Oliver Jordan Ressler’s comprehensive view highlights Cognitive Behavioral Therapy not as a passing fad, but as a scientifically grounded, practice-proven method reshaping mental healthcare. With a proven track record across disorders, a clear mechanism rooted in cognitive science, and growing accessibility, CBT stands as a model for effective, scalable therapy in the 21st century—where psychological transformation is both measurable and attainable.


Related Post

A Comprehensive Overview of Oliver Jordan Ressler’s Contributions to Modern Risk Analysis

How Tamara Tunie Unveiled the Secrets to Her Bliss: A Groundbreaking Insight into Inner Peace

Gimkit Join The Game Changer in Education – What ‘A’ for Student 2025 Really Means

Gary Burghoff Obituary

