Cat Bite: Swift Treatment & Rabies Vaccine Guide – Protect Your Pet and Public
Cat Bite: Swift Treatment & Rabies Vaccine Guide – Protect Your Pet and Public
When a cat suffers a bite—often from another feline or a stray—the risk of infection is significant, with rabies looming as the most dangerous consequence. Even minor punctures can introduce pathogens, making prompt intervention essential. Understanding the full scope of treatment options, wound management, and mandatory rabies vaccination is critical for cat owners, veterinarians, and public health officials alike.
This definitive guide distills the latest veterinary protocols into a clear, actionable resource for addressing cat bites effectively while preventing one of the deadliest zoonotic diseases. pouches the silent threat of cat bites: why rabies demands immediate attention A cat bite may appear superficial at first glance—a small red puncture or a slightly swollen area—but its hidden danger lies in the rapid transmission of bacteria, primarily *Pasteurella multocida*, along with potential rabies virus if the biting animal is suspected of being infected. Rabies, though preventable in most pets through vaccination, remains almost 100% fatal once clinical symptoms appear.
According to the World Health Organization, over 59,000 human rabies deaths occur annually, with animal bites—especially from cats and dogs—accounting for the majority. For cats, an untreated bite wound becomes a vector not only for local infection but a potential public health hazard. Immediate First Aid and Veterinary Treatment After a Cat Bite
Responding quickly to a cat bite failure to mitigate infection and prevent systemic spread.
Every cat bite should trigger a structured response:
- Secure the wound with sterile gauze, but avoid twisting or probing—this risks pushing bacteria deeper.
- Flush the wound thoroughly under running water for 5–10 minutes using an antiseptic solution such as diluted chlorhexidine or betadine, minimizing contamination.
- Control bleeding with gentle pressure; if it persists beyond 10–15 minutes, seek immediate veterinary care.
- Administer analgesic and anti-inflammatory treatment under professional supervision to manage pain and swelling without compromising healing.
- Apply a thin layer of broad-spectrum antimicrobial ointment, followed by a sterile, breathable dressing that allows moisture release.
- Schedule an urgent veterinary examination—early diagnosis prevents abscess formation, systemic infection, and long-term tissue damage.
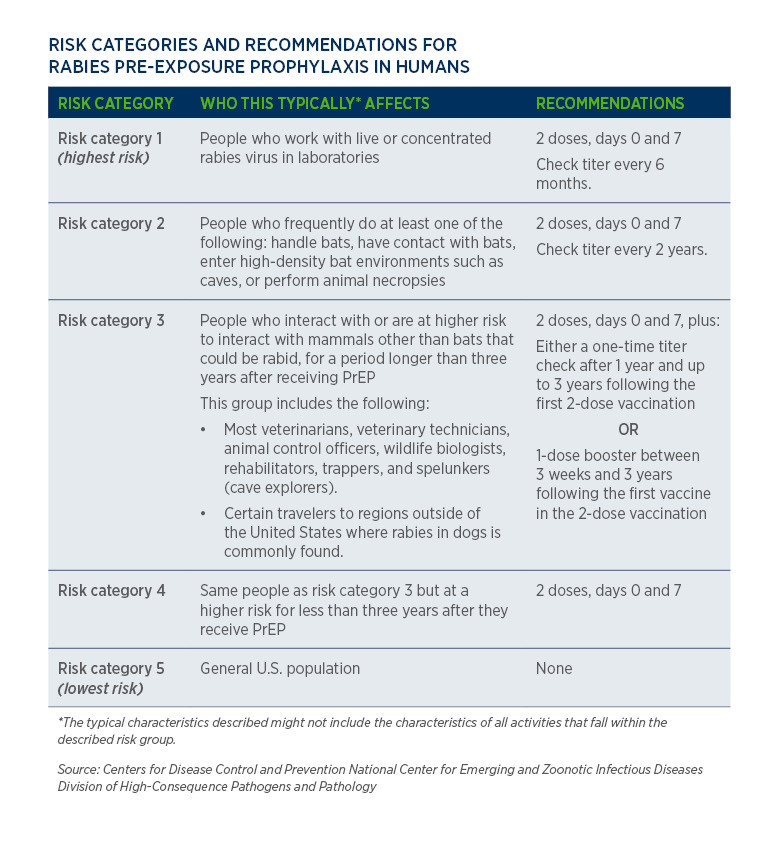
Understanding Rabies Risk and Post-Exposure Protocols
Rabies transmission through cat bites is rare but highly consequential.Only infected animals—especially strays or unveiled pets with unknown vaccination status—pose a threat. The rabies virus attacks the central nervous system, leading to fatal encephalitis, yet it remains 100% preventable with appropriate post-exposure prophylaxis. The CDCP (Centers for Disease Control and Prevention) stresses that proper wound management combined with timely rabies vaccination forms the cornerstone of protection.
In the event of exposure, immediately clean the bite area and consult a veterinarian or public health authority—especially in regions where stray cat populations thrive. For cats, the standard rabies vaccine protocol includes a core series initially, followed by annual or triennial boosters depending on local regulations and risk exposure. The World Animal Protection notes: “Maintaining up-to-date vaccination for cats is not only a medical mandate but a civic duty in rabies-endemic zones.” Vaccination: The Cornerstone of Prevention After Cat Bites
Vaccination remains the most effective shield against rabies, delivering high efficacy when administered correctly.
For cats, the typical protocol includes a primary series of two doses administered 3–4 weeks apart, with a third booster recommended annually or every three years based on risk level and vaccine type. In regions with strict wildlife exposure or frequent stray interactions, annual revaccination is strongly advised. The rabies vaccine triggers robust immune responses, producing neutralizing antibodies within 7–10 days.
Once vaccinated, cats develop near-complete protection, drastically reducing the risk of disease transmission. Veterinarians reinforce: “A cat’s rabies immunity is only as strong as its vaccination schedule—never delay findings from a bite.” For exposure incidents, pre-exposure vaccination primes the immune system effectively, while post-exposure vaccination—given within 48 hours of bite—eliminates the virus before neural invasion. Administering the vaccine promptly, concurrent with veterinary wound management, maximizes protective outcomes.
Quoting vaccine specialist Dr. Elena Morozov, “Combining immediate wound care with timely rabies immunization creates a nearly impenetrable defense system.” Common Complications and When to Escalate Care
Even with appropriate treatment, cat bite wounds may develop complications. Early signs include increasing redness, swelling, pain, warmth, and pus formation—indicating bacterial infection.
More severe outcomes include abscesses, deep tissue necrosis, or systemic sepsis if left untreated. Neurological symptoms such as aggression, paralysis, or fever suggest possible rabies exposure and demand emergency veterinary intervention. “If a cat bite begins healing but later swells, discharges, or shows fever—seek care immediately,” cautions Dr.
Maya Lin, emergency veterinary clinician. “Delayed recognition of infection or rabies progression can prove fatal.” Bloodwork, imaging, and serial wound assessments help monitor healing and detect silent threats early. Public awareness remains crucial: educating cat owners on bite symptoms, timing of treatment, and legal vaccination mandates helps prevent dangerous lapses.
In urban and rural settings alike, community engagement transforms individual action into collective resilience against rabies. Legal and Public Health Responsibilities: Beyond the Clinic
Post-bite care extends beyond submission to a veterinarian. In many jurisdictions, local health authorities require documentation of the bite, vaccination records, and sometimes quarantine or testing for cats with unknown immunization status.
This interface between clinical practice and public policy underscores a shared responsibility: preventing rabies outbreaks before they start. Cats regarded as “strays” or lacking vaccination credentials may trigger mandatory reporting and public health protocols, including controlled observation or euthanasia if rabid. Therefore, owners bear legal and ethical duty to act swiftly—recordings of wound care, vet visits, and vaccination logs become critical evidence in safeguarding both people and animals.
Professor Rajiv Nair, public health virologist, asserts: “Waste not; want not—every bite-reviewed cat bite is an opportunity to support broader disease control. Timely intervention upholds animal welfare, personal health, and community immunity.”
Even the most subtle feline aggression can unleash hidden threats—but with precise wound care, rapid veterinary assessment, and immediate rabies vaccine administration, risk transforms into control. Owners, veterinarians, and public health entities must move in unison: treat bite sites without delay, vaccinate with confidence, and remain ever-vigilant.
In doing so, we protect not only individual cats but the fragile web of human and animal health against one of the oldest and most deadly diseases on record.
:strip_icc()/how-long-are-rabies-shots-good-3385625_FINAL-b3b90b78675e4a9ca4102b405fecf74c.jpg)

Related Post

Eddy Funeral Home Jamestown, ND: A Cornerstone of Gentle Remembrance in Northwest Missouri’s Heartland

The Power of Precision: How Murray Bartlett Partner Revolutionizes Executive Communication and Brand Impact

Keyshia Cole’s Ethnicity: Shaping Identity in Hip-Hop and Beyond

How Ariana Greenblatts’ Parents The Young Shaped Her Art: The Power of Family Legacy in Identity

